On this page
- Part 1: Why should health services respond to victims of family violence?
- Part 2: What can health services do to respond to victims of family violence?
- National systems infrastructure
- Guideline, policy and documentation
- Resources
- Staff support
- VIP training
- Quality improvement and evaluation
- Evaluation and audit
- Definitions, Bibliography and Acknowledgements
Part 1: Why should health services respond to victims of family violence?
Health consequences of violence
Health consequences of violence
Rationale for a family violence intervention programme
- The magnitude of need: family violence is common, the cost of family violence is high in terms of the victim’s health and financially to the health service (Snively 1994).
- Health harm from abuse is cumulative, routine abuse enquiry identifies at-risk individuals and increases opportunities for early intervention.
- Experts, patients and purchasers support family violence intervention programmes.
- Ministry of Health family violence assessment and intervention guidelines are clearly endorsed by family violence agencies’ support programmes.
- Patients have identified that abuse enquiry is acceptable and that the health professional is someone who can support victims who disclose abuse (Freidman et al 1992, Koziol-McLain et al 2005).
- The Ministry of Health requires DHBs’ planning and funding teams to report on their responsiveness to family violence.
- The failure to implement a family violence intervention programme may lead to an unsatisfactory outcome. When a victim does not receive the level of support from the health service they expect, they may feel discouraged from further help-seeking. Without help, abused patients’ health deteriorates and the cost of their care rises (Campbell et al 1994).
- Additionally, as it becomes standard practice to respond to family violence, health organisations are likely to be criticised if they have failed to offer support to patients, especially following a homicide investigation.
Identifying the advantages and disadvantages of establishing or not establishing a programme may be beneficial when outlining rationale for the programme.
Contact the National VIP Manager for DHBs for further information and assistance.
Ministry of Health requirements
Ministry of Health requirements
Why does the health service need to offer family violence intervention?
Funding for DHBs is provided to support the implementation of the Ministry of Health Family Violence Assessment and Intervention Guideline.
This includes funding for a dedicated coordinator position to support programme establishment and implementation for child abuse and intimate partner violence assessment and intervention.
Knowledge of the acute and long-term consequences of trauma and violence continues to increase.
Violence and abuse cause significant and cumulative health harm – the longer violence and abuse continues the worse the mental and physical health harm.
Victims of violence use services at approximately three times the rate of people who are not victimised (Fanslow 2004, Krug 2002; Koss, Koss & Woodruff 1991).
The Adverse Childhood Experiences (ACE) study suggests that being a victim of child abuse and/or witnessing partner abuse is linked to serious health problems in adulthood (Felitti et al 1998; Edwards et al 2005) including not only injuries but also effecting sexual and reproductive health, mental health and increasing the risk of chronic disease.
Early intervention provided by health professionals’ identification and support of child and adult victims is important to reduce health harm, social harm and health service utilisation.
The FVIAG intervention is highly acceptable to patients, increases help-seeking behaviour, and reduces medium term incidence of violence (Koziol-McLain et al 2005, McFarlane et al, 1998 and 2000, Muellman et al 1999).
Working to foster safe, stable and nurturing relationships between adults and children and healthy and respectful relationships between intimate partners are fundamental aspects of supporting health (FVAIG 2016).
International recognition of the significance of family violence
The seriousness of family violence is recognised by international organisations, conventions and documents, including:
National recognition of the significance of family violence for government sectors (excluding health)
The New Zealand Government recognises family violence as a priority issue, as shown in:
- Children’s Action Plan (external link)
- Vulnerable Children Act 2014 (external link)
- Te Rito: New Zealand Family Violence Prevention Strategy (2002) (external link)
National recognition of the significance of family violence for the health sector
The New Zealand Government recognises family violence as a priority issue, as shown in:
- the Ministry of Health’s Statement of Intent 2015 to 2019 (external link)
- the New Zealand Health Strategy 2016 (external link)
- the Primary Health Care Strategy (external link)
- He Korowai Oranga: Māori Health Strategy (external link) – refreshed 2014
- the Crown Funding Agreement with DHBs (external link)
Health professionals
Health professionals have more access to families than almost any other service provider. Health professionals have the opportunity to identify abuse early, provide immediate support and offer referrals, which could prevent serious harm or death.
Health professionals have a professional responsibility to act as an advocate for victims of abuse (Nursing Council of New Zealand 2001).
Victims
Victims feel that health professionals should be able to provide support and offer intervention options (Campbell et al 1994, Koziol-McLain et al, 2005).
New Zealand victims of violence who have experienced the health service intervention are strongly positive about the impact of receiving support and information, and assistance in help seeking (Koziol-McLain 2005, DSAC 2005). Women find being questioned in health care settings regarding their experience of IPV to be both acceptable and appropriate (Feder et al 2009; Koziol-McLain et al 2008; MacMillian et al 2009).
Victims have identified that when a health professional does not ask about their safety or screen for violence, they can feel helpless, discouraged (Campbell et al 1994) and less likely to seek help in the future (Head and Taft 1995). Doing nothing can reinforce a patients feelings of humiliation and can compound damage to their sense of self worth (Jecker 1993).
Victims will usually disclose violence if asked in a safe, non-judgmental way within the context of a health assessment (Freidman et al 1992, Koziol-McLain et al, 2005).
Ethical considerations
Ethical considerations
Health professionals have an ethical responsibility to diagnose appropriately.
- The ethical principle of beneficence suggests that health professionals have a professional responsibility to diagnose and treat abuse rather than to merely address physical symptoms, also considering the psychological, social and spiritual dimensions of health.
- The ethical principle of non-malfeasance suggests that health professionals’ failure to recognise family violence has the potential to lead to further injury and/or inappropriate or harmful treatment. For example, if abuse is the underlying reason for a health issue and it is not identified, then any treatment may be ineffective and even detrimental (McLeer and Anwar 1997; Spinola et al 1998).
Health professionals who adopt an abuse enquiry practice within their usual health assessment increase opportunities to provide early intervention and education on family violence.
Part 2: What can health services do to respond to victims of family violence?
How a successful programme fits in everyday practice
Evaluations of Violence Intervention Programme highlight that a systematic approach can achieve organisational and attitudinal change.
Central to this is developing training programmes, practice protocols, standardised documentation, support processes, posters, monitoring and evaluation (Campbell et al 2001).
The systems that support the VIP are both national and those recommended for DHB VIP.
National systems infrastructure



DHB systems infrastructure

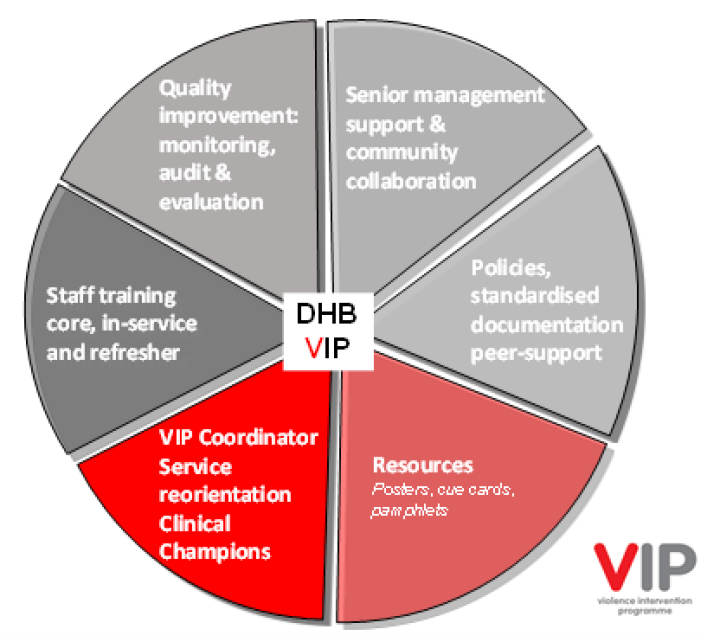
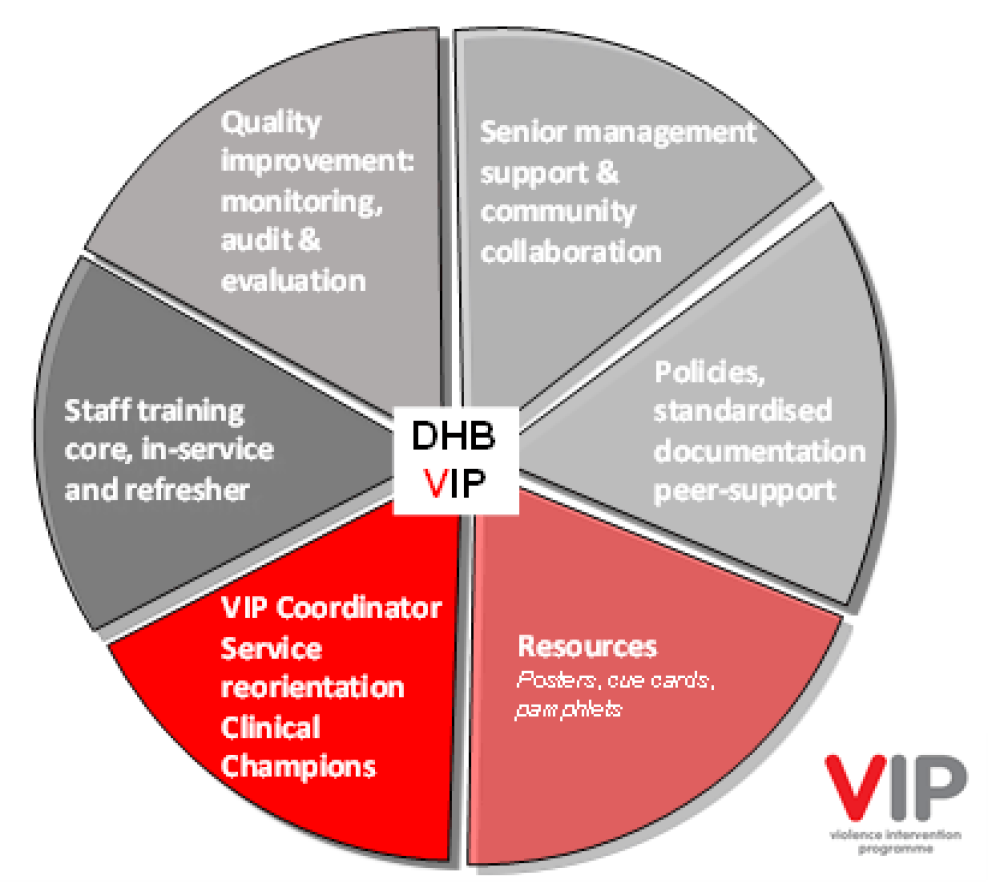
The pie chart above depicts the ‘systems check’ for each service to ensure that all support processes are established, prior to beginning the VIP. These mutually reinforcing activities include:
- senior management support and community collaboration
- guidelines and policies
- resources including cue cards, posters, pamphlets and flowcharts
- funded VIP coordinators including staff support, mentoring and supervision
- training
- quality improvement, monitoring, audit and evaluation.
Reorienting services and starting where success is likely
A key message that can be shared with staff is that Violence Intervention Programme is core to a health professional role.
Health professionals have a responsibility to identify family violence, assess health and risk, and refer victims of abuse because the prevalence of violence and its health impact make it our business.
Most health professionals are taught to fix a problem, but this does not work in partner abuse intervention.
Partner abuse intervention is not a ‘quick fix’; instead we are successful when we empower the person experiencing abuse. Offering the intervention is the intervention.
A Violence Intervention Programme, which includes sensitive enquiry questions, requires an environment that is ready and receptive to change. Start where the programme is wanted and where success is likely to occur.
Guideline, policy and documentation
Health sector Violence Intervention Programme policy development
1. Principles of a policy or procedure
Policies are intended to support staff practice.
A policy should define the broad areas it covers, for example, generic family violence policy or separate policies for child abuse, intimate partner violence, and elder abuse and neglect.
A policy needs to align with National Guidelines, professional standards and legislative requirements (eg, Vulnerable Children Act 2014).
The policy must meet the needs of the services it relates to. The steering/reference group process must manage collaboration, consultation and completeness, including community agency collaboration and participation, which includes Māori and Pacific consultation.
The policy should cover:
- scope
- principles
- responsibilities (ie, of the DHB, service/department/unit and employee)
- procedures for practice, including a clear intervention process with a referral pathway (this may include a flow chart delineating the process)
- relevant legislation
- associated documentation
- review/audit processes.
A guide to establishing a Violence Intervention Programme policy is available to download in Word and PDF format:
- Guide to Establishing a Violence Intervention Programme Policy (Word, 29KB) [DOC, 29 KB]
- Guide to Establishing a Violence Intervention Programme Policy (PDF, 11KB) [PDF, 11 KB]
2. Example of policies
Intimate Partner Violence Policy
This policy provides all district health board (DHB) staff with a framework to identify and manage intimate partner violence.
The policy also provides guidelines for the development of unit specific policies relating to identification and management of intimate partner violence.
- Intimate Partner Violence Intervention Policy (Word, 844KB) [DOC, 844 KB]
- Intimate Partner Violence Intervention Policy (PDF, 1.1KB) [PDF, 1.1 MB]
Child Abuse and Neglect Policy – Management of
This policy provides DHB community and hospital-based staff with a framework to identify and manage actual and/or suspected child abuse and neglect.
It recognises the important role and responsibility staff have in the accurate detection of suspected child abuse and/or neglect, and the early recognition of children at risk of abuse and adults at risk of abusing children.
- Child Abuse and Neglect Policy – Management of (Word, 620KB) [DOC, 620 KB]
- Child Abuse and Neglect Policy – Management of (PDF, 1.4MB) [PDF, 1.4 MB]
3. Examples of standardised documentation
For examples of standardised documentation identified in the Family Violence Assessment and Intervention Guideline: Child abuse and intimate partner violence 2016, see:
- Intimate Partner Violence (IPV) Assessment and Intervention Documentation form (Word, 65KB) [DOCX, 65 KB], (PDF, 501KB [PDF, 501 KB])
- Acute Post Strangulation documentation form – see appendix L (pages 114–115) of the Family Violence Assessment and Intervention Guideline: Child abuse and intimate partner violence (external link).
Here is an example of coded intimate partner violence question as presented on the emergency department assessment form:
|
IPV |
RE |
Y |
+ve |
-ve |
N |
Initial |
Key:
IPV= Intimate Partner Violence
RE = Routine Enquiry
Y = Yes, question asked
+ve = abuse disclosed
-ve = no abuse disclosed
N = No, question not asked
Initial = Initial of staff member asking the question
4. Privacy of documentation
Individual DHBs need to develop a process to manage patient information, recognising the following principles.
- A standardised form must be used to encourage methodical documentation of the abuse disclosure.
- The information must be stored securely to ensure that the disclosing persons information cannot be accessed by their partner.
- The information should be recorded so that it can be communicated between services (see Privacy Discussion document below).
Managing the Privacy of Documentation Recording Intimate Partner Violence Disclosures: A discussion document
This discussion document was written to study the process of recording intimate partner violence disclosures.
Three principles require consideration when developing a system of recording intimate partner violence disclosures.
- Developing a method for maintaining the privacy of disclosed information
- Maximising the victim’s safety
- Ensuring the information is communicated appropriately, thereby minimising risk to the patient and the organisation.
The document considers 3 areas.
1. Confidentiality of patient information especially from the perpetrator of abuse
While every effort is made to protect the disclosed information while the patient is in clinical areas, this cannot always be controlled.
There is concern that a partner might access this information if the documentation form were filed in the general notes, and this might place the victim/patient at risk of retaliation. While every effort is made to avoid this, there will be times when patients carry their own notes to appointments.
2. Communication between health services of patient intimate partner violence risk
There is a requirement to communicate information between health care services. A system is necessary to ensure that when intimate partner violence has been identified by one service, the information is made available to all other services.
This is based on the principle of taking action to ensure the information is communicated to appropriate services, rather than being held in isolation and potentially placing the patient at risk (Commissioner for Children 2000).
3. Recording abuse information disclosed by mothers of child patients
The guideline recommends routine enquiry questioning mothers of all children presenting to health services.
This raises the issue of where to store the documentation of intimate partner violence disclosed, because the mother’s information should not be held in the child’s records.
This recognises the mother’s right to privacy and the risk of the partner accessing the child’s notes if that partner is a legal guardian.
For more information email the National VIP Manager.
Resources
Staff require appropriate resources to support the Violence Intervention Programme.
Resources support and educate staff every day, acting as a conscious and subconscious reminder of the need to include routine enquiry in their clinical practice.
Resources for staff need to be available before the programme is launched in the service/department/unit. Such resources include:
- readily available policies to direct practice
- cue cards for staff, with framing questions
- community directories
- flow charts in care areas
- posters
- victim resources, including community agency resource cards, safety plan sheets and pamphlets on agencies
- assessment forms amended to record the routine enquiry process and outcome. This information may need to be coded to ensure a victim's partner does not inadvertently view the disclosure, which may put the victim at risk.
Go to Health professional resources to access Ministry of Health resources.
Staff support
Internal champions
Internal champions are clinically credible staff who include Violence Intervention Programme into their practice and advocate introducing intimate partner violence interventions into service/department/unit practice.
Staff who adopt the role of internal champion support change by:
- talking informally with colleagues about the importance of Violence Intervention Programme in practice
- supporting colleagues to develop competence in VIP practice.
A champion will encourage staff to ask patients about intimate partner violence in formal and informal ways.
This may include reminding staff at the beginning of a shift to ask all female patients during that shift about intimate partner violence, reminding staff if they note that the routine enquiry hasn't been completed yet or initiating a conversation between staff about the importance of intimate partner violence interventions within practice.
A team of champions within the service/department/unit supports the Violence Intervention Programme and expands the resources available for staff as they begin to adopt the interventions in their practices.
Mentor programme
What is mentoring?
Mentoring is an important part of the internal support that is needed to implement the DHB Violence Intervention Programme.
Mentoring takes place in a cooperative and supportive relationship that is based on mutual trust and respect. A professionally experienced and competent worker provides:
- active encouragement of trained staff to use their new skills in practice
- opportunity for staff to share their new experiences with others
- guidance and support when difficulties arise
- clarification and reinforcement of Violence Intervention Programme policy (procedures and protocols)
- direction regarding further networks, resources and personnel if a problem lies beyond their area of expertise or experience.
Skills and abilities related to Violence Intervention Programme
Mentors should be competent in the following skills and knowledge in Violence Intervention Programme:
- dynamics, indicators and impacts of intimate partner violence
- the DHB policy (procedures and protocols), including support and referral
- managing confidentiality and documentation
- using routine enquiry questions and offering intimate partner violence interventions.
Supervision
Clinical supervision is a vital component of the Violence Intervention Programme to ensure staff and patient safety is optimal.
Clinical supervision must be easily accessible for staff within their clinical setting and should incorporate 3 components.
- Maintenance of professional standards.
- Development of the practitioner through self-reflective learning in a supportive environment and expansion of practitioner awareness.
- Support of the practitioner (Bond and Holland 1994).
Supervision should be offered after any disclosure of abuse to ensure the staff's learning and support can be maximised.
Confidentiality must be maintained, except where patient or staff safety is at risk.
VIP training
1. Principles of training
Collaboration is key to Violence Intervention Programme – engage community agencies on the teaching team, for their expertise and so staff can be directly informed of the agency’s role (Fanslow et al 1998).
Training ensures that all staff have the necessary knowledge and skills to integrate the Violence Intervention Programme in their practice.
Training should take place once all policies, documentation, staff support processes, referral pathways and resources are available and prior to launching routine enquiry in any service.
Training needs to be endorsed by management, and it needs to be mandatory to be effective.
Training works best when provided across a whole health service.
Training should be in a dedicated time, lasting for between 4 and 16 hours (Campbell et al 2001; Fanslow et al 1998).
2. Strategic approach to training
A DHB VIP training plan that includes introduction, core, refresher, advanced and peer support training:
- Violence Intervention Programme Training Plan (Word, 87KB) [DOC, 87 KB]
- Violence Intervention Programme Training Plan (PDF, 430KB) [PDF, 430 KB]
A brief one-hour introduction to intimate partner violence and child abuse and neglect that covers prevalence, impact, the rationale for routine enquiry and barriers and enablers for change. This introduction session is valuable because it:
-
introduces the concept of intimate partner violence and child abuse and neglect intervention and enables staff to have time to consider its relevance to their practice prior to training
-
introduces intimate partner violence and child abuse and neglect as a legitimate health issue
-
recognises that, given the prevalence, there will be staff that have personal experience of intimate partner violence and child abuse and neglect. The delivery of the session and the timing offers staff time to seek any support required before attending the full training day. This reflects the DHB commitment to safe practice.
Ideally this introduction would occur at least a month before the full training day.
The full Violence Intervention Programme training day should discuss:
- the epidemiology of intimate partner violence and child abuse and neglect and the effects on all persons experiencing the abuse
- theories and dynamics of intimate partner violence and child abuse and neglect
- why and how to routinely enquire for intimate partner violence and what to do if the person discloses abuse
- strangulation identification, assessment, management and response
- child abuse and neglect identification, assessment and referral including principles and practice
- the role of community agencies for intimate partner violence, child abuse and neglect
- needs and responsibilities to Māori incorporating the 12 kaupapa identified in the Family Violence Assessment and Intervention Guideline - Child abuse and intimate partner violence 2016 (FVAIG 2016)
- professional dangerousness with regard to intimate partner violence and child abuse and neglect intervention; responses that can lead to unsafe practice
- resources available to support VIP
- focusing on the 6 step intervention model:
- Identify (Routine Enquiry)
- Acknowledge the disclosure (Validation and support)
- Assess health and risk
- Discuss safety
- Refer and follow up
- Document.
Role-play abuse identification and intervention, using scenarios applicable to attendees clinical practice (eg, specific service/department/unit focus).
Annual refresher training may be required to update staff and ensure practice standards are maintained.
Refresher training can be tailored to the needs of the service/department/unit, or it can take the form of a generic presentation, depending on demand and staff members’ levels of confidence with Violence Intervention Programme.
In-service training is delivered as short targeted service updates for small groups/ individual staff members. The content of the in-service training package is specific to the service it is being presented to.
It should be developed to address areas of the programme where improvement potential has been identified from ward/service area audit results. Additionally it may include programme updates that need to be communicated to staff.
Advanced training may be required for some staff in each service who can act as mentors, or to develop internal champions to advocate the programme among colleagues.
While training can be generic, grouping attendees by seniority, speciality, profession and designation may help target the training to an appropriate level of clinical practice.
3. Training evaluations
Evaluations of the sessions using a pre- and post-teaching design offer an opportunity to assess understanding before training and demonstrate training effectiveness.
A VIP Quality Improvement resource kit that includes pre- and post- training evaluation is available.
Please contact National VIP Manager for DHBs for further information.
4. Maximising training
Training alone is not enough; ongoing support, including one-to-one support for staff, is required to achieve and sustain change.
Management mandating training for staff is a key success factor. This is a visible demonstration of management’s commitment to the programme and demonstrates management has prioritised the programme.
5. Violence Intervention Trainers
| Resource | Focus | Contact |
|---|---|---|
| SHINE Safer Homes in New Zealand Everyday |
Contract by the Ministry of Health for health-specific training; training for professionals and the community; DV-free workplace support; education programmes for schools; refuge services, crisis advocacy, a 24 hour helpline; perpetrator programmes | Email: enquiries@2shine.org.nz Phone: (09) 81 |
Quality improvement and evaluation
Evidence for the intervention
What outcomes can you expect from introducing a violence intervention programme? How do you know you are making a difference?
- Customer satisfaction rates will increase, and victims will give positive feedback about the health professional offering family violence intervention.
- Rates of routine enquiry and victim identification will increase across services.
- Rates of referrals from health services to community agencies will increase.
- The DHB’s score on the Ministry of Health Audit of DHB responsiveness to family violence will improve.
Longer-term outcomes may include:
- decreased utilisation of health services by victims of family violence
- reduced long-term rates of family violence
- children growing up in safer families
- breaking the cycle of violence.
How can the quality of family violence intervention be measured and maintained?
To ensure the quality and safety of the intervention supervision/peer support should be provided for health professionals when they first begin family violence intervention (after a disclosure of abuse). This allows staff to:
- assess their standard of practice during self-reflective learning
- receive the necessary emotional and professional support regarding practice.
Pre- and post-teaching evaluations can assess how much staff understand about family violence intervention before and after the training session.
This helps the training coordinator assess where additional support is necessary to ensure quality intervention is offered.
Audits should be conducted regularly to assess:
- the staff’s knowledge and understanding of family violence intervention policies
- intimate partner violence routine enquiry rates, adherence to policy/procedures and standards of documentation.
Staff should be surveyed regularly to assess the barriers that need to be addressed and to identify potential opportunities for family violence interventions within their practice.
Quarterly feedback from the community agencies who receive referrals from the DHB is an effective way of monitoring that the quality and quantity of referrals has increased since inception of a family violence intervention programme.
Quality improvement activities such as conducting PDSA cycles can identify and measure specific and targeted programme performance (eg, identification by PDSA regarding aspects of the programme performing well in one area may be replicated, implemented and subsequently measured by utilising a PDSA cycle in another area).
Evaluation and audit
Evaluation and monitoring are pivotal aspects of the implementation of a programme, when the intention is to achieve and sustain change (Campbell et al 2001; Grimshaw et al 1999).
Evaluations should have practical value or be useful to the target audience, for example the coordinator of the family violence intervention programme and or steering group.
Evaluations and audit can be useful for many reasons including:
- evaluations can influence decision-making regarding programme implementation, for example indicating need for refresher training or increased resources
- evaluations can provide updates on implementation progress in accordance with performance indicators that are supplied to senior management
- evaluations provide an opportunity for stakeholders to feed into the change process. For example, asking staff about the barriers and enablers to routine enquiry and the strategies to address these issues or asking community agencies to report on the quality and quantity of referrals received
- clinical audits and evaluation processes can support change of staff attitude and organisational culture when provided as feedback. Staff are informed and learn about how the family violence intervention programme is being implemented, the impact on practice and the outcomes
- evaluation provides useful information to the staff and conveys a message of collaboration
- evaluation and audit offers a process that engages staff in the process
- well defined evaluation processes ensure a 360-degree feedback loop is in place.
A simple audit tool can be used to record audit results. If you would like further information or assistance regarding development of audit tools and resources please contact the National VIP Manager for DHBs.
Audit templates
Terms of reference for a clinical audit can provide a guideline for audit implementation.
- Terms of Reference for a Clinical Audit (Word, 70KB) [DOCX, 70 KB]
- Terms of Reference for a Clinical Audit (PDF, 332KB) [PDF, 332 KB]
Contact the National VIP Manager for more information.
Evaluation reports
Go to Reports on Violence Intervention Programmes (VIP) in district health boards (external link).
Definitions, Bibliography and Acknowledgements
Definitions - Family violence
Definitions - Family violence
-
Child
Unborn children and children aged 0 to 14 years. Note that Oranga Tamariki Act 1989 Children’s and Young People’s Well-being Act 1989 covers young people up to their eighteenth birthday.
-
-
Child abuse
The harming (whether physically, emotionally or sexually), ill treatment, abuse, neglect or serious deprivation of any child, or young person (Section 2(1) Oranga Tamariki Act 1989 Children’s and Young People’s Well-being Act 1989).
-
-
Child emotional/psychological abuse
Any act or omission that results in impaired psychological, social, intellectual and/or emotional functioning and development of a child or young person.
-
-
Child protection
Activities carried out to ensure the safety of the child in cases where there is abuse or risk of abuse.
-
-
Child sexual abuse
Any act or acts that result in the sexual exploitation of a child or young person, whether consensual or not.
-
-
Family violence
Violence or abuse of any type, perpetrated by one family member against another family member, including child abuse, partner abuse and elder abuse.
-
-
Intimate partner violence (also called partner abuse)
Physical or sexual violence, psychological/emotional abuse, or threat of physical or sexual violence that occurs between intimate partners.
-
-
Neglect
Any act or omission that results in impaired physical functioning, injury and/or development of a child or a young person, including physical and medical neglect, neglectful supervision, abandonment and refusal to assume parental responsibility.
-
-
Physical abuse
Acts of violence that may result in pain, injury, impairment or diseases, may include hitting, choking or in any way assaulting another person and also under/over medicating.
Physical abuse usually results in visible evidence of bruising, fractures, burns, lacerations, etc, though the difference between accidental injury and abuse can be slight and require expert investigation.
Child physical abuse is any act or acts that may result in inflicted injury to a child or young person.
-
-
Routine enquiry
Enquiry, either written or verbal, by health care providers to an individual about their personal history of partner abuse, child abuse or neglect. Routine questioning of all individuals, or specified categories of individuals about abuse.
-
-
Young person
14–18 years old.
-
(Family Violence Intervention Guideline: Child abuse and intimate partner violence 2016.)
Bibliography
Bibliography
Bailhache M, Leroy V, Pillet P, et al. 2013. Is early detection of abused children possible?: a systematic review of the diagnostic accuracy of the identification of abused children. BMC Pediatrics 13: 202.
Bond M, Holland S. 1994. Developmental supervision in health visiting. Health visitor, 67, 11. 392–3.
Campbell J. 1994. Child abuse and wife abuse: the connections. Maryland Medical Journal 43(4): 349–50.
Campbell JC, Coben JH, McLoughlin E, Dearwater S, Nah G, Glass N, Lee D, Durborow N. 2001. An evaluation of a system-change training model to improve emergency department response to battered women. Academic Emergency Medicine 8(2): 131–8.
Campbell J, Pliska M, Taylor W, Sheridan D. 1994. Battered women’s experiences in the emergency department. Journal of Emergency Nursing 4(20): 280–8.
Carroll-Lind J, Chapman J, Raskaukas J. 2011. Children’s perceptions of violence: the nature, extent and impact of their experiences. Social Policy Journal of New Zealand 37: 1–13.
Commissioner for Children. 2000. Final report on the investigation into the death of James Whakaruru. Wellington: Office of the Commissioner for Children.
Christian CW, Scribano P, Pinto-Martin JA. 1997. Pediatric injury resulting from family violence. Pediatrics 99 (2): e8. URL: http://pediatrics.aappublications.org/content/99/2/e8.full (external link) [Accessed 28 August 2002].
Doctors For Sexual Abuse Care 2005. Women’s experiences of domestic violence: An audit of consultations from four GPs, Unpublished report for the Ministry of Health 2005.
Edelson J 1999. The overlap between child maltreatment and women’s battering. Violence Against Women; 5: 134–54.
Edwards VJ, Anda RF, Dube SR, et al. 2005. The wide-ranging health consequences of adverse childhood experiences. In Kendall-Tackett K, Giacomoni S (eds). Victimisation of Children and Youth: Patterns of abuse, response strategies. Kingston, NJ: Civic Research Institute.
Family Violence Death Review Committee. 2014. Fourth Annual Report: January 2013 to December 2013. Wellington: Family Violence Death Review Committee.
Fanslow J, Norton R, Spinola C. (1998). Indicators of assault-related injuries among woman presenting to the emergency department. Annals of Emergency Medicine 23(3): 331–63.
Fanslow J and Robinson E. 2004. Violence against women in New Zealand: prevalence and health consequences. New Zealand Medical Journal 117(1206).
Feder G, Ramsay J, Dunne D, et al. 2009. How far does screening women for domestic (partner) violence in different health-care settings meet criteria for a screening programme? Systematic reviews of nine UK National Screening Committee criteria. Health Technology Assessment 13: 1–113.
Felitti V, Anda R, Nordenberg D, Williamson D, Spitz A, Edwards V, Koss M, Marks J. 1998. Relationship of childhood abuse and household dysfunction to many of the leading causes of death in adults: the adverse childhood experiences (ACE) study. American Journal of Preventative Medicine 14(4): 245–58.
Freidman LS, Samet JH, Roberts MS, Hudlin M, Hans P. 1992. Inquiry about victimization experiences: a survey of patient preferences and physician practices. Archives Internal Medicine 152: 1186–90.
Grimshaw J, Shirran E, Thomas R, Mowatt G, Fraser C, Bero L, Grilli R, Harvey E, Oxman A, Thomson M, Baker R, Donald A, Dunning M, Firth-Cozens J, Hodgkin P, Sowden A. 1999. Effective health care: getting evidence into practice. Effective Health Care Bulletin 5(1): 1–16.
Head C, Taft A. 1995. Improving General Practitioner Management of Women Experiencing Domestic Violence: A study of the belief and experiences of women victims/survivors and GPs. Victoria: Hawthor, 1–33.
Jecker NS. 1993. Privacy beliefs and the violent family. JAMA 296(6): 776–80.
Koss, M, Koss, P, Woodruff, W. 1991. Deleterious effects of criminal victimisation on women’s health and medical utilisation. Archives Internal Medicine, 151: 342–7.
Koziol-McLain, Giddings L, Rameka M, Fyfe E. Women’s Perceptions of Partner Violence Screening in Two Aotearoa Healthcare Settings: “What took You so Long”. Unpublished evaluation report for the Ministry of Health 2005.
Koziol-McLain J, Giddings L, Rameka M, et al. 2008. Intimate partner violence screening and brief intervention: experiences of women in two New Zealand Health care settings. Journal of Midwifery & Women’s Health 53: 504–10.
Krug E, Dahlberg L, Mercy J, Zwi A, Lozano R, World Report on Violence and Health World Health Organization Geneva 2002.
Langley J, Martin J, Nada-Raja S. 1997. Physical assault among 21-year-olds by partners. Journal of Interpersonal Violence 12: 675–84.
Lievore D, Mayhew P. 2006. The Scale and Nature of Family Violence in New Zealand: A review and evaluation of knowledge. Wellington: Crime and Justice Research Centre, Victoria University.
McFarlane J, Parker B, Soeken K. 1996a. Abuse during pregnancy: associations with maternal health and infant birth weight. Nursing Research 45(1): 37–42.
McFarlane, J., Parker, B., Soeken, K., Silva, C., & Reel, S. 1998. Safety behaviours of abused women after an intervention during pregnancy. Journal Obstetric Gynecology Neonatal Nursing, 27(1), 64–9.
McFarlane, J., Soeken, K., and Wiist, W. An evaluation of interventions to decrease intimate partner violence to pregnant women. Public Health Nursing, 17(6), 443–451, 2000.
McKibben L, DeVos E, Newberger E. 1989. Victimization of mothers of abused children. Pediatrics 84: 531–5.
McLeer SV, Anwar RAH. 1987. The role of the emergency physician in the prevention of domestic violence. Annals of Emergency Medicine 16: 1155–61.
MacMillan HL, Wathen CN, Jamieson E, et al. 2009. Screening for intimate partner violence in health care settings: a randomised trial. JAMA 302(5): 493–501.
Maxwell G. 1994. Children and Family Violence: The unnoticed victims. Occasional paper number 3. Wellington: Office for the Commissioner for Children.
Maxwell G, Barthauer L, Julian R. 2000. The Role of Primary Care Providers in Identifying and Referring Child Victims of Family Violence. Wellington: Office for the Commissioner for Children.
Minister of Health. 1998. Child Health Strategy. Wellington: Ministry of Health.
Minister of Health. 2016. The New Zealand Health Strategy: Future Directions 2016. Wellington: Ministry of Health.
Minister of Health. 2001. The Primary Health Care Strategy. Wellington: Ministry of Health.
Minister of Health and Associate Minister of Health. 2002. Refreshed 2014. He Korowai Oranga: Maori Health Strategy. Wellington: Ministry of Health.
Ministry of Health. 2016. Family Violence Assessment and Intervention Guideline: Child abuse and intimate partner violence. Wellington: Ministry of Health.
Ministry of Health. 2015. Statement of Intent 2015–2019. Wellington: Ministry of Health.
Ministry of Social Development. 2002. Te Rito New Zealand: Family violence prevention strategy. Wellington: Ministry of Social Development.
Ministry of Social Development. 2014. Children’s Action Plan. Wellington: Ministry of Social Development.
Ministry of Social Development. 2014. Vulnerable Children’s Act. Wellington: Ministry of Social Development.
Muellman et al. 1999. Family Violence, Ministry of Health Requirements
Murphy C, Paton N, Gulliver P, Fanslow J. 2013. Understanding connections and relationships: Child maltreatment, intimate partner violence and parenting. Issues paper 3. New Zealand Family Violence Clearinghouse.
Raphael B. 2000. Domestic violence. The healthcare sector could become agents for change. The Medical Journal of Australia 159: 513–4.
Snively S. 1994. The Economic Cost of Family Violence. Wellington: Coopers and Lybrand.
Spinola C, Stewart L, Fanslow J, Norton R. 1998. Developing and implementing an intervention: evaluation of an emergency department pilot on partner abuse. Evaluation & the health professions 21(1): 91–118.
Acknowledgements
Acknowledgements
The Ministry of Health would like to acknowledge the significant contributions DHBs have offered in developing this guideline.
The generous offers of material and editing advice from DHB coordinators of family violence intervention programmes (child and partner abuse) are also greatly appreciated.